Debunking common mpox myths
sommthink // Shutterstock
Debunking common mpox myths
A worker’s hand uses a pipette to test sampoles in a lab
The CDC on May 15 issued an official health update warning people to be on the lookout for an uptick in cases of mpox, formerly known as monkeypox. This warning came after 21 cases of mpox were confirmed in the Chicago metro area from April into early May of this year.
As is the case with most widely discussed scientific topics, misinformation on the mpox virus is everywhere. False narratives were especially common during the widespread outbreak of the disease in the summer of 2022, ranging from labeling mpox a “gay disease” to claims that it is a secret bioweapon.
Truth can seem hard to come by when the news changes so rapidly amid a firehose of updated information. Some of the best ways to combat misinformation include seeking additional primary sources that don’t rely on the first source you encounter; looking for opinionated statements hidden among “facts;” being diligent in avoiding confirmation bias—the tendency to seek out information that supports what you already believe to be true; and following a story for multiple days to allow the narrative to develop more completely.
Stacker compiled a list of myths about mpox and investigated their viability using news, scientific, and government reports.
Additional places to find reliable, science-based information include the Centers for Disease Control and Prevention, the World Health Organization, the U.S. Food and Drug Administration, the U.S. Department of Health and Human Services, and the American Medical Association.
![]()
Stacker
Myth: Mpox isn’t widespread and won’t affect me
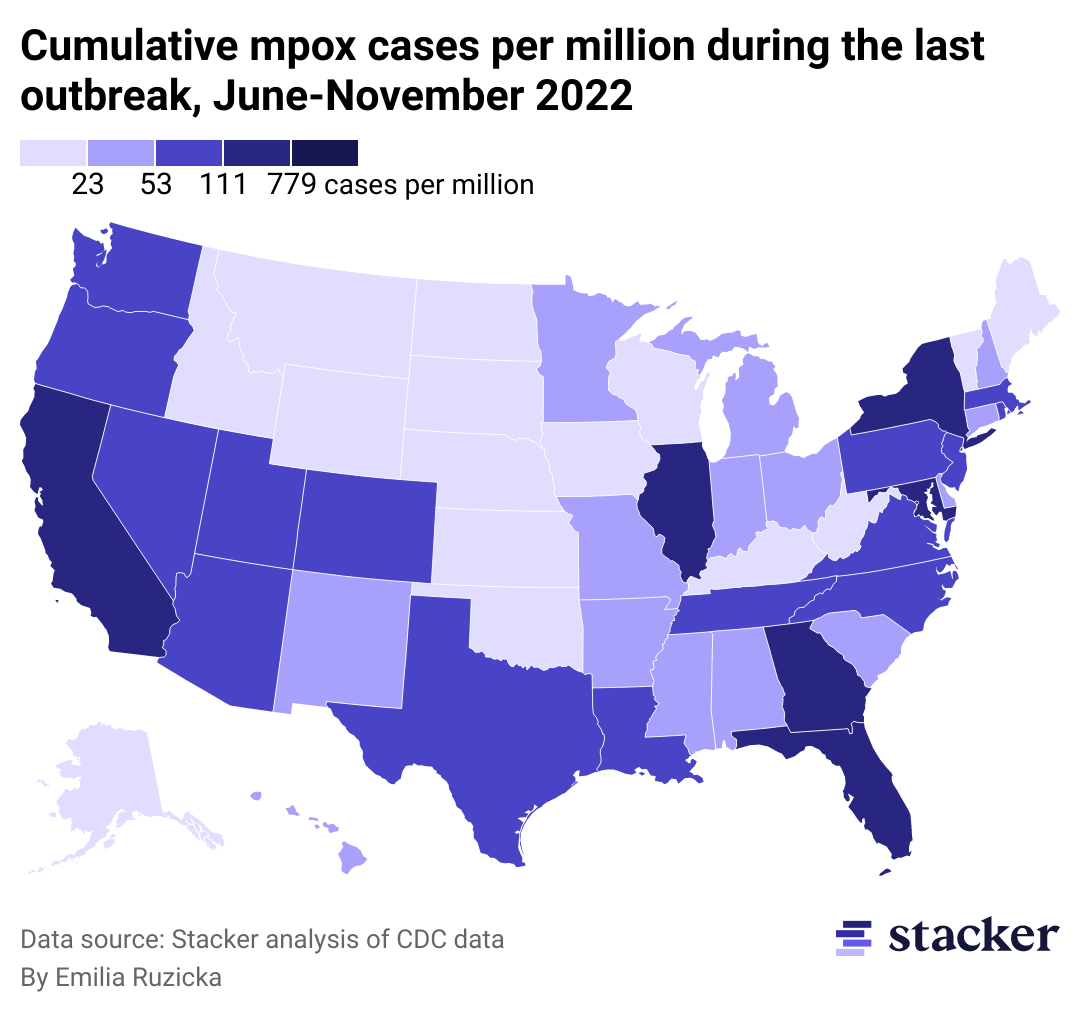
A map of the US showing cumulative mpox cases from June to November 2022
All states and Washington D.C. have recorded at least one case of mpox since early July 2022. Wyoming announced its first case on Aug. 22, 2022, making it the last state to do so. California had the most confirmed cases overall during the last outbreak at 5,768 as of June 9, 2023.
Though not every city, state, or region was a hot spot, the disease spread across the country, and the CDC has released guidance to help people protect themselves and others in public and shared spaces. Anyone can contract mpox, so taking the recommended precautions for your own health is the best defense against illness, especially as the CDC warns of a possible renewed outbreak.
Smith Collection/Gado // Getty Images
Myth: Mpox is a new disease
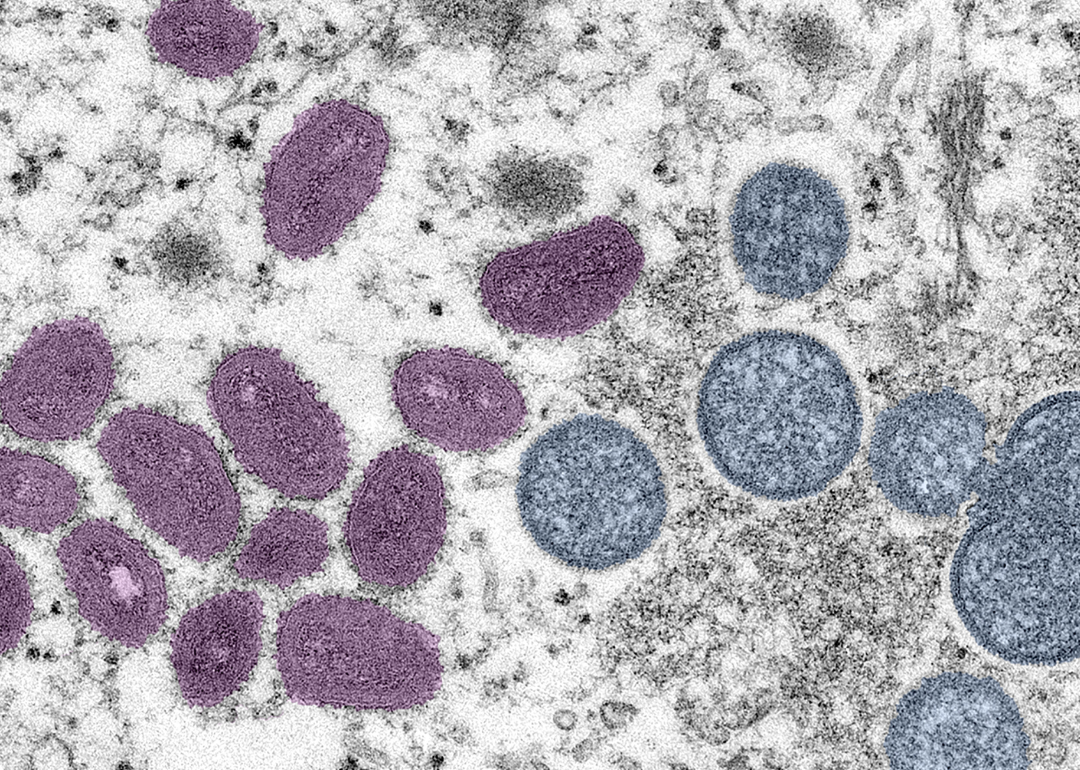
Electron microscopic image if monkeypox virion
The mpox virus was identified in humans for the first time in 1970, according to the WHO. A 9-month-old boy contracted mpox in a rural area of the Democratic Republic of Congo, where smallpox had already been eliminated for two years. Since then, two large outbreaks have occurred in Africa in 1996-1997 and 2017, and the virus has been detected across 11 African countries.
Outside of Africa, the first known mpox case was in 2003 in the U.S. That case was traced back to a pet prairie dog that had been infected, leading to more than 70 human infections. Additional countries that have experienced mpox outbreaks outside of Africa are Israel in 2018, Singapore in 2019, and the U.K. throughout 2018-2022.

Mike Roemer // Getty Images
Myth: Mpox is an STI
Man having an appointment with an STD specialist in a clinic
Though two people who engage in sexual contact may spread the mpox virus to each other if one is already infected due to being in close skin-to-skin contact, mpox is “not a sexually transmitted disease in the classic sense,” according to Northwestern Medicine infectious diseases expert Dr. Robert L. Murphy. Murphy states that because mpox is not spread via sex-related fluids like semen, it cannot be called a sexually transmitted infection. However, engaging in close physical contact with another person is one of the ways that mpox can spread, which is why it can appear to spread similarly to some STIs.
Other experts warn that the misinformation about mpox being an STI could make people feel like it won’t impact them if they have a committed partner or don’t have sex, which is not the case. Experts also worry that labeling mpox as an STI may cause people with symptoms to feel ashamed and not report their infection due to stigma, which could help the disease spread further.
Stacker
Myth: Mpox only affects the LGBTQ+ community
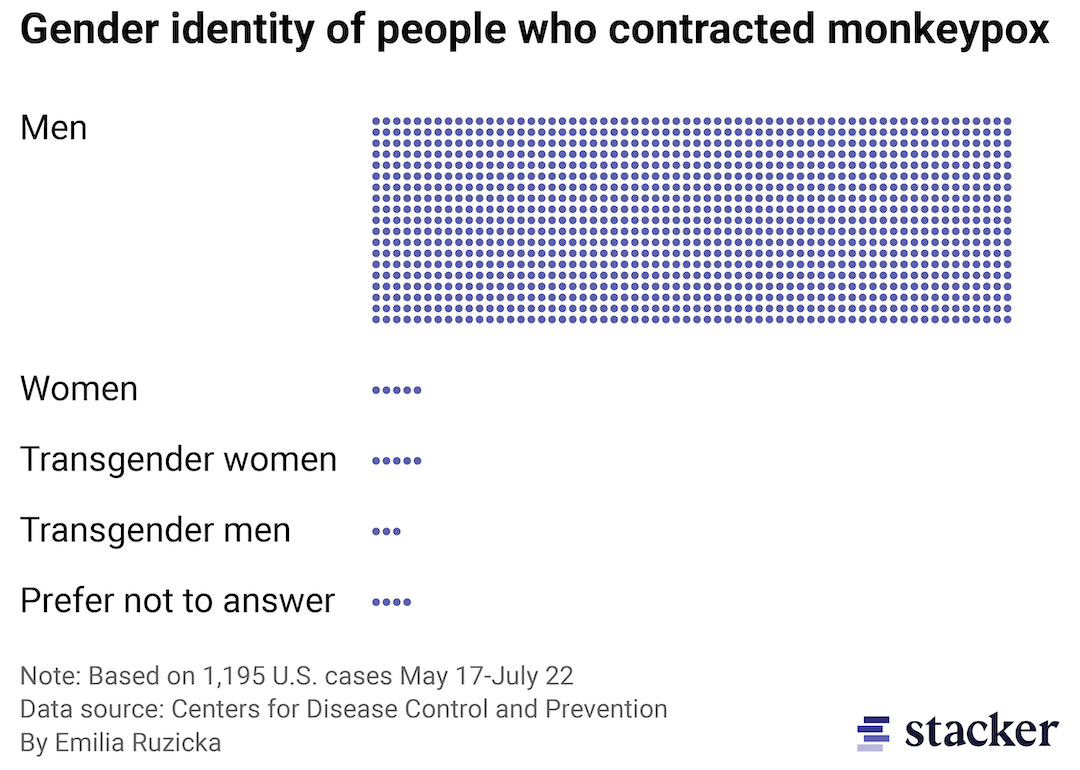
Bar chart made of dots depicting the gender identity of people who contracted monkeypox in the U.S.
According to a CDC study, “[a]mong U.S. [mpox] cases with available data, 99% occurred in men, 94% of whom reported recent male-to-male sexual or close intimate contact.” While mpox is currently disproportionately affecting the LGBTQ+ community, anyone can get it regardless of age, gender, or sexual orientation. Currently, the virus is primarily spreading among men who engage in sexual activity with other men because the community is more insular resulting in more frequent contact, not because of their sexual orientation or practices.
Current conversations about mpox are reminiscent of the stigmatization of HIV patients in the late 20th century. This misinformation could result in decreased access to resources in communities that need them the most and increased stigmatization of and hate towards members of the LGBTQ+ community.

Drazen Zigic // Shutterstock
Myth: Mpox spreads like COVID-19
A woman in a protective mask shops in a market
Throughout the COVID-19 pandemic, wearing masks and other facial coverings became common because the coronavirus is primarily transmitted through respiratory droplets in the air. Essentially, the tiny virus particles attach themselves to small drops of water or other material and travel through the air from one person to another.
In contrast, the mpox virus primarily spreads through extended direct contact with another infected person. The rash, scabs, and body fluid that are the hallmarks of mpox are especially adept at spreading infection. If such fluids or other body matter infected with the virus are left on surfaces, those surfaces can also spread the infection if a person spends a prolonged period of time in contact with them.

Karen Ducey // Getty Images
Myth: Mpox spread to humans from monkeys
Two research scientists at work in lab
Despite the fact that mpox did not infect humans until 1970, the virus was first discovered in a group of primates in 1958, which prompted scientists to name the disease “monkeypox.” However, just because primates can be carriers of mpox does not mean that current or historical outbreaks were directly caused by primate-to-human transmission.
According to the CDC, mpox can be carried by a “wide range of mammal species, including monkeys, anteaters, hedgehogs, prairie dogs, squirrels, shrews, and dogs.” The species of the original disease carrier for the 2022 outbreak in the U.S. is unknown. There has been at least one instance of mpox transmission from humans to a dog, so the CDC recommends that infected individuals avoid contact with their pets.
Stacker
Myth: Mpox is a mild disease
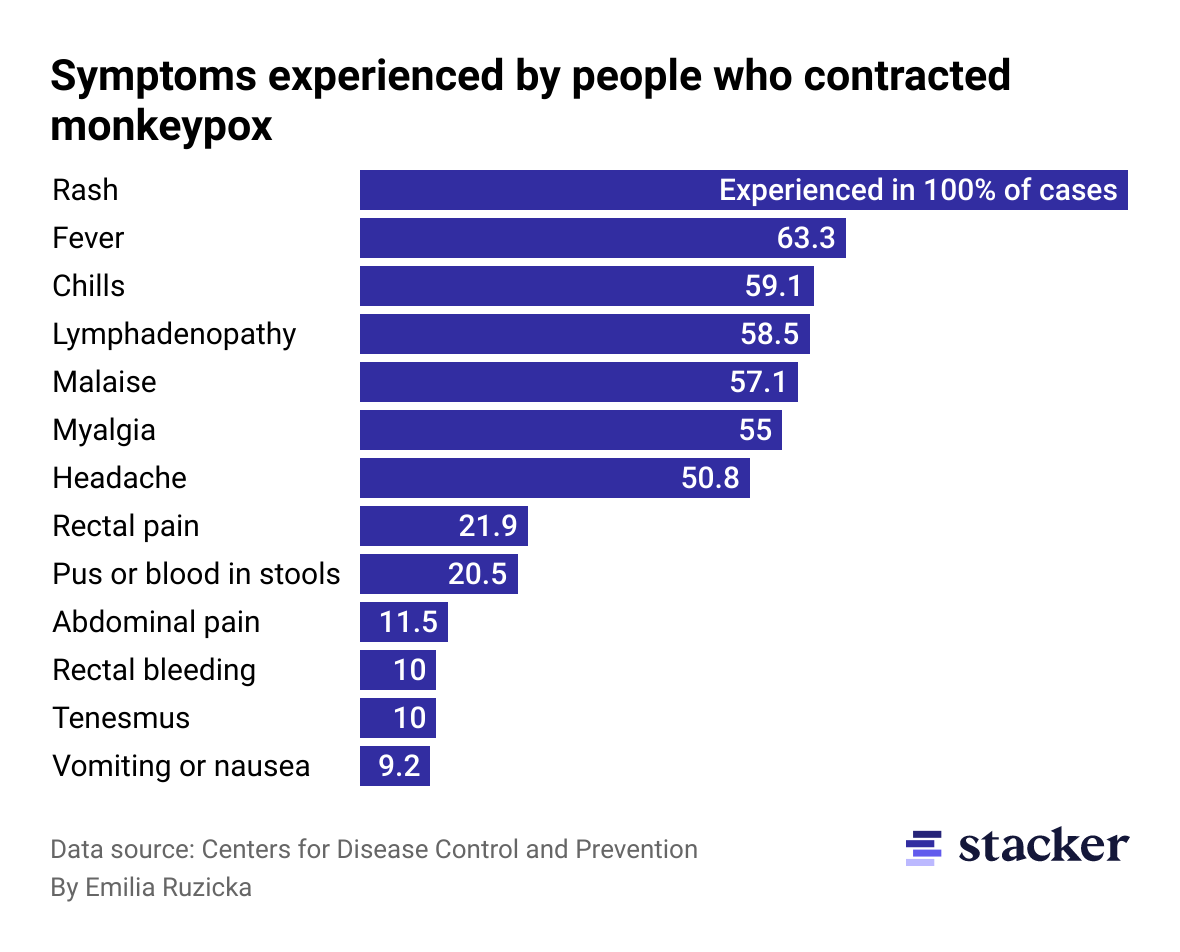
Bar chart depicting symptoms experienced by people who contracted monkeypox in the U.S.
Because diseases with high death rates have been at the forefront during the COVID-19 pandemic, mpox can seem low-stakes in comparison. On Aug. 30, 2022, the first death by a presumed positive mpox case was recorded in Texas. Historically, about 15% of people with the disease have died.
However, just because a disease is typically less than fatal does not mean precautions should be ignored. Common mpox symptoms include rash, fever, and swollen lymph nodes, and symptoms typically last 2-4 weeks. The rashes, or “pox,” caused by the virus can be incredibly painful and leave permanent scars.
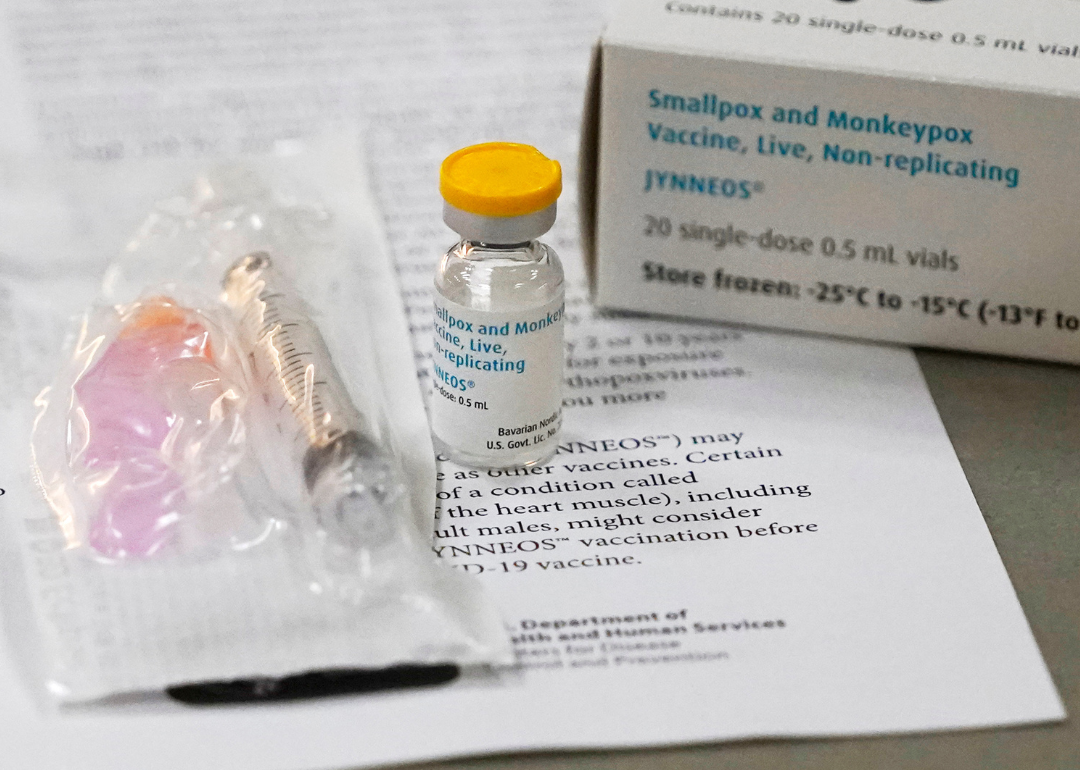
David Joles/Star Tribune via Getty Images
Myth: The Mpox vaccine is new and unresearched
Vial of monkeypox vaccine and information paperwork at clinic
The Jynneos vaccine is currently the only FDA-approved vaccine to protect against mpox. It requires two doses, four weeks apart, for the best protection. It was originally developed to protect against smallpox but has been updated to better fight the mpox virus.
According to experts, the mpox and smallpox viruses share about 85% of their genetic material. As a result, people who received the smallpox vaccine before it was no longer required in the U.S. in 1972 may have slightly increased immunity. The CDC states that the smallpox vaccine is most effective at preventing smallpox infection within 3-5 years after vaccination, so there may be a similar effect for mpox.

Mario Tama // Getty Images
Myth: The mpox vaccine is available and anyone can get it
Monkeypox vaccination appointment sign with QR code and health workers at clinic
Mpox vaccines were administered to states by the federal government for distribution. Every state is responsible for its own vaccine rollout practices, and during the summer 2022 outbreak, many were forced to limit who could receive the vaccine due to supply shortages. As a result, the federal government offered a new vaccine strategy that includes administering smaller doses of the vaccine. The CDC is working with local health authorities to help administer vaccines and spread mpox awareness at a variety of Pride events during the month of June.
The CDC recommends those who “have been exposed to [mpox] and people who may be more likely to get [mpox]” get vaccinated, including those who have been identified as close contacts of someone with an mpox infection. To find a clinic where you can receive a free vaccine, use the CDC’s Mpox Vaccine Locator.
