From battlefields to bedsides: The evolution of modern EMTs

Found Image Holdings // Getty Images
From battlefields to bedsides: The evolution of modern EMTs
Light trails from a 1950s Cadillac ambulance driving on a road.
Just six decades ago, you had a better chance of surviving a gunshot wound during the Vietnam War than by being treated in an ambulance on the way to the hospital in the U.S.
It’s hard to imagine American cities without the blaring, screeching presence of ambulances, but in fact, emergency response services are a relatively new phenomenon. Up until the mid-1960s alone, first responders were often funeral home workers, who transported patients in the same hearses that would later be used during their funerals.
At the same time, a National Academy of Sciences report pointed out that, in 1965, “accidental injuries killed 107,000, temporarily disabled over 10 million, and permanently impaired 400,000 American citizens at a cost of approximately $18 billion.” The death toll and economic costs were overwhelming, but a potential low-hanging solution was available: Paramedics from the Vietnam War frontlines would provide a blueprint for first responders, who could be dispatched to the scene of an injury—and fast.
What started as an experimental solution took hold, and went through decades of advancement, quickly adapting to increasing medical shortages, new inventions, and critical needs.
Today, the modern EMT profession has expanded to include standard EMTs, paramedics, advanced EMTs, and emergency medical responders, encompassing different levels of skill and specialization. There are an estimated 269,000 EMTs and paramedics working in the U.S. as of 2022, and the field is projected to grow by 5% by 2032—faster than other industries on average.
But the history of EMTs is not just a story of medical advancements. Over just half a century, the evolution of the role has been a story of socioeconomic development, city planning, and war, just to name a few influences. For instance, the advent of highways increased both the need and opportunity for the EMT profession. The first EMTs were, in fact, a group of Black men in Pittsburgh who were trained on the world’s first comprehensive paramedics course and saw high success rates—but the program was nixed in favor of replacing them with an all-white squadron.
Medical Technology Schools used historical and medical sources to delve into the five biggest moments in the evolution of modern EMTs, beginning with their formation for military assignments and continuing today. Read on to learn about the surprising origins of one of America’s most high-stakes professions.
![]()

MPI // Getty Images
Early 1860s-1950s: EMTs begin on the battlefield
Members of the Fifth Regiment New York Volunteers conduct an ambulance drill.
The very beginnings of the EMT can be traced all the way back to the Civil War, an event that produced an unprecedented level of battlefield trauma and required a large-scale and organized effort to attend to the injured.
In 1862, Major Jonathan Letterman established the U.S. Ambulance Corps, first within the Army of the Potomac and eventually throughout the entire Union Army. This enabled the treatment of injured soldiers during battle, rather than waiting until open fire had ceased.
This model was expanded upon during World War I, when soldiers were able to summon medical attention on the battlefield using signal boxes. After the war ended, volunteers began to comprise the first civilian emergency responders, largely made up of fire departments and even undertakers.
It was landmark publications about CPR in the late 1950s and ’60s, however, that provided the impetus for emergency response services to make the leap from volunteer work to a legitimate profession. As articles laid out the best practices for cardiopulmonary resuscitation, the American Heart Association began to train physicians in CPR, paving the way for EMTs to learn as well.

H. Armstrong Roberts/ClassicStock // Getty Images
1960s: A white paper makes the dangers of roads clear
Two ambulance EMTs with woman on stretcher in front of brick suburban house.
By the 1960s, there was a nationwide shortage of registered physicians, and moreover, much of their time was taken up performing relatively elementary tasks that could be more quickly performed by less advanced personnel. Compounding this was the advent of the National Highway System, which meant an increase in vehicle injuries.
A landmark moment in the evolution of emergency medical services was the publication of a 1966 white paper, “Accidental Death and Disability: The Neglected Disease of Modern Society,” which had been put together by the National Academy of Sciences. The paper alerted President Lyndon B. Johnson to the startling fact that in 1965 alone, more Americans were killed in road accidents than in the Korean War.
Largely thanks to the report, the government mobilized to design an emergency response system, and returning medics from the Vietnam frontlines provided a blueprint to follow, which included their medevac transport protocols.
In 1969, the first national standardized curriculum for the emergency medical technician was published, signaling the beginnings of the modern civilian EMT.

H. Armstrong Roberts/ClassicStock // Getty Images
1960s-1970s: The EMT gains recognition as a profession in its own right
Emergency personnel loading a stretcher with patient into an ambulance at night.
Once the job of an EMT was introduced, the role spread rapidly, and by the end of the 1970s was recognized as a legitimate profession (rather than an offshoot of the work of firefighters or undertakers). Pivotal in this development was the Highway Safety Act of 1966, which included mandating the standardization of training for EMS workers, as well as developments to emergency transport services, including the installation of portable defibrillators in ambulances.
It didn’t take long for the EMS profession to spread in popularity, and in 1973, the EMS Systems Act was introduced, creating over 300 emergency service systems nationwide and reserving funding for future growth.
Around this time, physicians began to specialize in emergency medicine for the first time, with the first residency training program opening in 1972 at the University of Cincinnati. Within three years, that first program had ballooned to 32 different residencies across the country. More trauma centers also opened nationwide.
H. Armstrong Roberts/ClassicStock // Getty Images
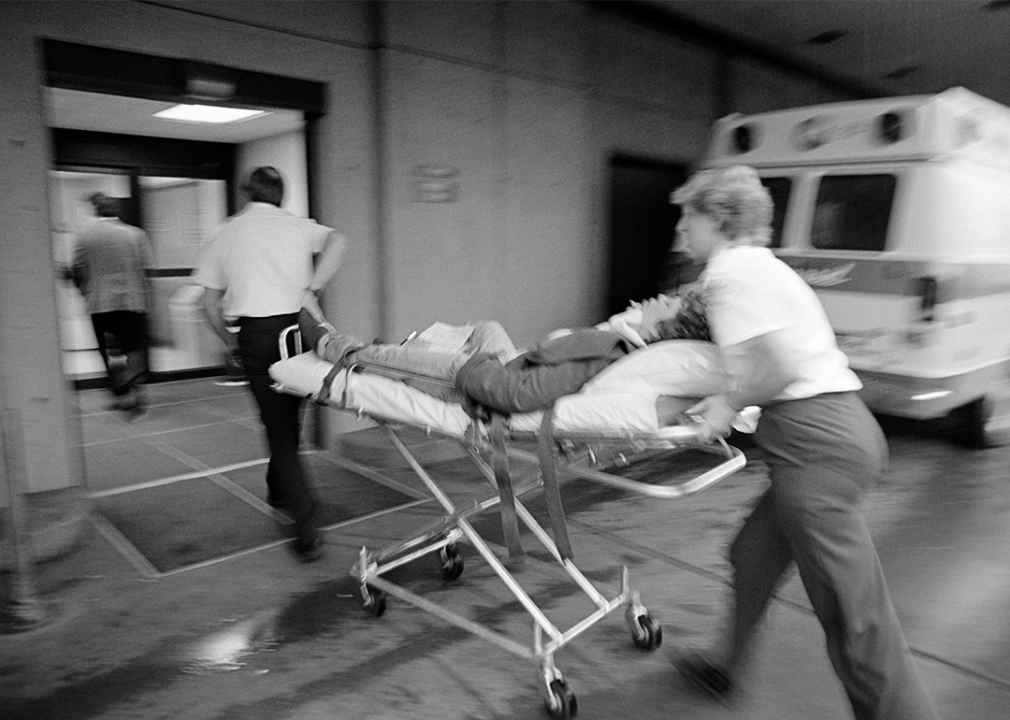
1970s-1980s: Emergency services become standardized—and sanitized
EMT team rushing a patient on a stretcher into the hospital.
Once the EMS role became nationally recognized, it began to go through several rounds of refinement to grow into the profession we know today. The National Highway Safety Act in 1966 also established the country’s inaugural Department of Transportation, which along with the National Highway Traffic Safety Administration, played a central role in standardizing curriculum, training, and standards for EMTs.
By the early 1970s, EMTs had become so widespread that it was necessary to distinguish a new role: the paramedic, who took on more advanced medical operations while allowing EMTs to perform baseline tasks.
In 1971, the first certifying exam for EMTs was undertaken by 1,520 individuals.
By the 1980s, emergency medical services began to expand beyond only treating adult trauma episodes to include addressing chronic diseases and pediatrics as well. It was also around this time that it became standard for emergency medical personnel to wear gloves and masks to protect against pathogens, a development that was at least partially spurred by fears surrounding the AIDS epidemic.

Scott Eisen // Getty Images
1980s-Today: New challenges for EMTs in a post-COVID world
A first responder wearing a face mask loads a patient into an ambulance.
Today, the modern EMT is facing a new shift in scope and identity in the wake of the COVID-19 pandemic. The shortage in medical personnel post-pandemic includes emergency medical technicians, who have been similarly overstretched and overwhelmed in caring for patients. For instance, many EMTs are grappling with shortages in available emergency room capacity, leading to extensive “wall time” spent waiting for patients to be checked in. This also means an ambulance is out of service until the patient can finally be admitted to the ER.
More positively, the same medical developments that are being considered for brick-and-mortar services are also being adapted to emergency services, including the possibility of expanding emergency services to include telehealth. Some EMS systems are now offering alternative destination options for emergency treatment facilities, and some cities are expanding EMT services to include mental health emergencies rather than dispatching police.
As the EMS profession continues to evolve and expand, so too does public appreciation for this historic, risky role: In 2018, the National EMS Memorial Foundation was commissioned to plan a permanent memorial to emergency medical service workers in Washington D.C.
Story editing by Carren Jao. Copy editing by Tim Bruns.
This story originally appeared on Medical Technology Schools and was produced and
distributed in partnership with Stacker Studio.
